Patients presenting with chest pain: Differential diagnoses
23rd June 2021
11 misdiagnoses in acute asthma in adults in the emergency department
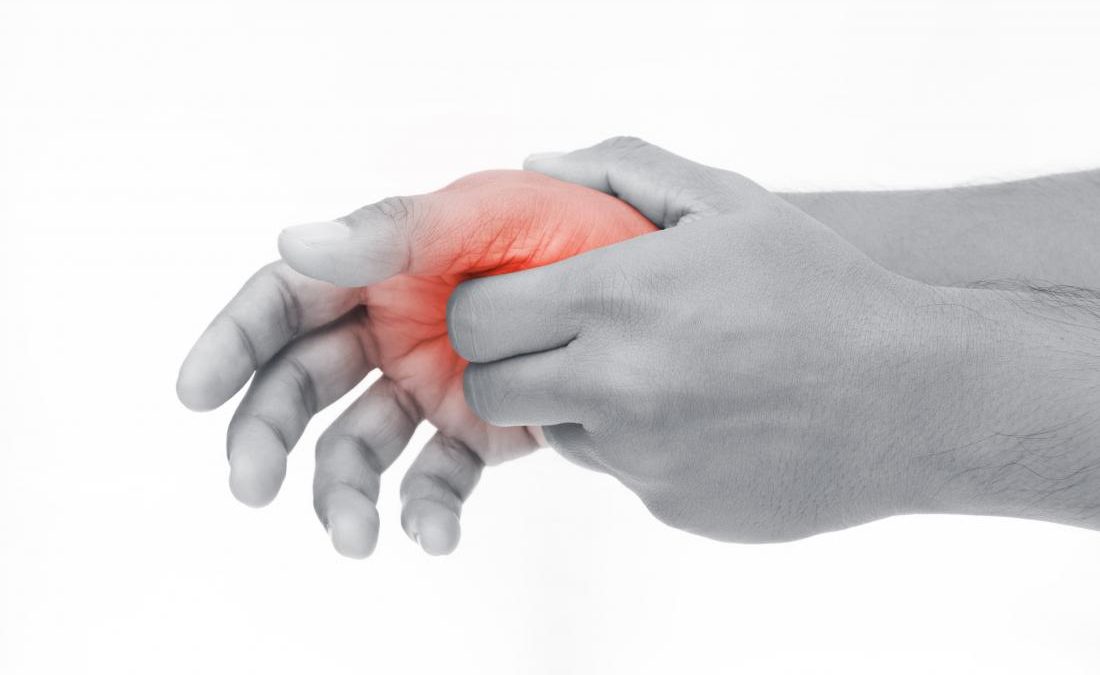
5th July 2021Tenosynovitis can be broadly defined as inflammation of a tendon and its respective synovial sheath. Tendons are the cords of tissue that hold muscle to bone. They help us to control actions such as grasping, lifting, running and jumping.
Tenosynovitis is most commonly seen in the wrist, hands and feet but can also occur in the shoulders, upper arm, lower arm and knee.
Tenosynovitis can be caused by injury, illness and repeated motion.
What is tenosynovitis with De Quervain’s and what are the causes?
Tenosynovitis with De Quervain’s occurs in the thumb. It is inflammation of the sheath that tends to be responsible for thumb movement.
The causes of tenosynovitis with De Quervain’s are often not clear. Overuse of the thumb tendons, particularly through repetitive actions, is often a causal factor, as is a sprain.
Patient presentation with tenosynovitis
Tenosynovitis can be infectious or non-infectious. Infectious forms can onset rapidly and be progressive. Common pathogens such as staphylococci and streptococci should not be overlooked in patients presenting with tenosynovitis that is suspected to be caused by infection.
An ED clinician should examine a patient’s medical history, lifestyle, occupation and functional status. Handedness should be enquired after to determine any increased risk of repetitive use as a cause. Smoking status, drug use, and the presence of peripheral vascular disease, diabetes mellitus, immunosuppression and renal disease may also be risk factors.
Some people are thought to be at greater risk of tenosynovitis. This can be those who work in roles that involve a variety of repetitive actions. It might include assembly line workers, office workers, tradespeople, dentists and musicians. Athletes can also be prone to tenosynovitis.
Accurate diagnosis by manoeuvring the hand and identifying the precise location of maximal tenderness is paramount. Radiographic assessment can rule out fracture depending on the patient’s presentation, age and history. MRI is not routinely used in diagnosis.
Patients with tenosynovitis with De Quervain’s
Patients with tenosynovitis with De Quervain’s will usually present complaining of radial wrist pain, discomfort from thumb movements and tenderness over the first dorsal compartment. There may be a thickening of the radial styloid.
The condition is common in mothers who have infants aged 6 to 12 months due to repetitive lifting. Daycare workers and others who work with babies or young children may also be affected.
Diagnosis, common misdiagnosis and overlooked conditions
It isn’t always clear what causes tenosynovitis so it can be overlooked or misdiagnosed, particularly in patients where risk factors are not necessarily obvious. Tenosynovitis conditions are often misdiagnosed as sprains.
Tenosynovitis with De Quervain’s can be more straightforward to diagnose. This is most often done by Finkelstein’s Test. It is performed by placing the thumb in the palm of the hand, making a fist around it then flexing the wrist inwards in the direction of the little finger. If the patient reports that pain is worse at the base of the thumb, then the result is considered to be positive.
Care should be taken by the practitioner not to confuse Finkelstein’s Test with Eichoff’s Test (which is a similar technique). Eichhoff’s Test may produce false-positive results, while a skilled medic performing Finkelstein’s Test is unlikely to achieve such a result.
The risks of non-diagnosis or missed diagnosis
Infectious tenosynovitis can result in damage to the tendon and surrounding structures if not diagnosed and treated promptly. It may require surgical debridement and washout, and sometimes amputation.
If untreated, non-infectious tenosynovitis can result in long-term pain and disability.
A failed or missed diagnosis of tenosynovitis with De Quervain’s can cause permanently restricted movement, or the sheath can burst which can require extensive and lengthy additional treatment.