Why Ask For Help?
16th November 2020
Unexplained Syncope –Investigation in the Emergency Department
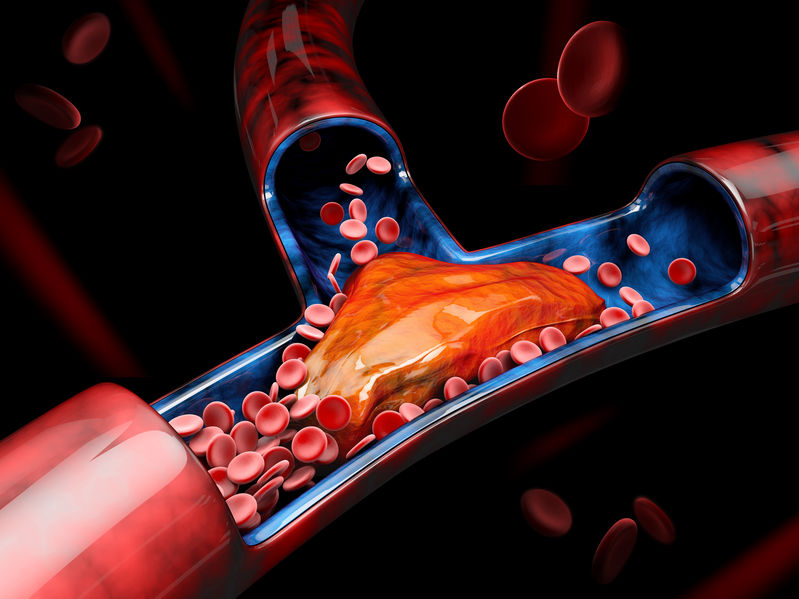
1st December 2020The disease process of venous thromboembolism (VTE) manifests as deep vein thrombosis (DVT) which often leads to pulmonary embolism (PE) if blood clots travel to the lungs. PE can be deadly if undetected, therefore it is imperative that the Emergency Department (ED) clinician understand the correct procedures for diagnosing and managing suspected DVT/PE.
There are several confounding factors that can prevent an accurate diagnosis of DVT/PE:
- symptoms are non-specific and can mimic other serious ailments (e.g. chest pain, tachycardia and shortness of breath);
- presence risk factors (age, recent surgery, oral hormonal therapy) is not a clear indication of presence or absence of VTE;
- and disease progression an vary wildly (in some cases symptoms last for days and in others the sudden onset of symptoms leads to a precipitous decline).
It is essential that the healthcare provider arrive at a quick diagnosis so that the correct treatment may be administered. For this, one needs to maintain a high index of suspicion for DVT/PE and understand how to rule out other ailments.
As with any patient presenting to the ED, conducting an initial assessment and obtaining a thorough history are essential first steps. The detailed history is especially important as asking the right questions in the right way can help rule out a DVT/PE diagnosis. For example, exertion dyspnea (shortness of breath) is a common sign of DVT/PE, however, most people experience shortness of breath at some point. It is important for the clinician to obtain details about the circumstances in which the patient has experienced dyspnea to understand if it is a cause for concern. A patient reporting dyspnea accompanied by fatigue should raise the degree of suspicion for a DVT/PE diagnosis. Another common indicator of DVT/PE is leg pain or swelling. As patients with DVT/PE often do not present in distress, the clinician should pay attention to subtle signs and symptoms that may indicate some type of venous thromboembolism. (Streiff et al., 2016)
Two common tools utilized in determining the pretest probability of DVT/PE are the Wells criteria for DVT and PE and the PERC (Pulmonary Embolism Rule Out Criteria). These should be utilized after the initial assessment has raised suspicion of a possible VTE diagnosis. These tools consider factors such as heartrate (>100 bpm), blood oxygenation (<95%), unilateral leg swelling, recent trauma or surgery, recent period of immobilization, oral hormonal therapy and age over 50 years. Used in conjunction with the patient’s history, these factors can help a physician decide if further testing is necessary.
NICE provides a useful chart to help in the decision process when PE/DVT is suspected. If the pretest probability is high, NICE recommends running the D-dimer test. While waiting for the lab results, it is recommended that the patient receive interim anticoagulation treatment. If the patient’s Wells score is higher or equal to 2 points, then NICE recommends imaging tests to be conducted: a proximal vein leg ultrasound for patients with suspected DVT or a CT pulmonary angiogram (CTPA) for those with suspected PE. If either the D-dimer or the scan are positive, further investigation and treatment should be considered. For confirmed DVT the recommended course is outpatient treatment with enoxaparin sodium (i.e. Clexane) and continued monitoring.
A PE diagnosis is easy to miss in patients with comorbidities that can explain the symptoms being experienced. At the same time, not using the Wells score can lead to overestimating a healthy patient’s risk for PE based on their symptoms. This leads to unnecessary testing and exposure to radiation when the Wells score could have ruled out a PE diagnosis in a healthy person. At the same time, it is important not to mistake absence of tachycardia, or other obvious risk factors, for the absence of PE. A normal heart rate upon assessment does not necessarily rule out PE, nor does absence of obvious risk factors. According to one 2003 study, 25%-50% of patients with VTE do not have readily identifiable risk factors.
The main lesson here is that appropriate guidelines should be followed regardless of first impressions when DVT/PE is suspected. VTEs provide many diagnostic challenges in the ED due to the many confounding factors that can interfere with an accurate diagnosis. However, following accepted procedures relating to pretest assessment, testing recommendations and management with anticoagulants will yield the best outcome for the patient.