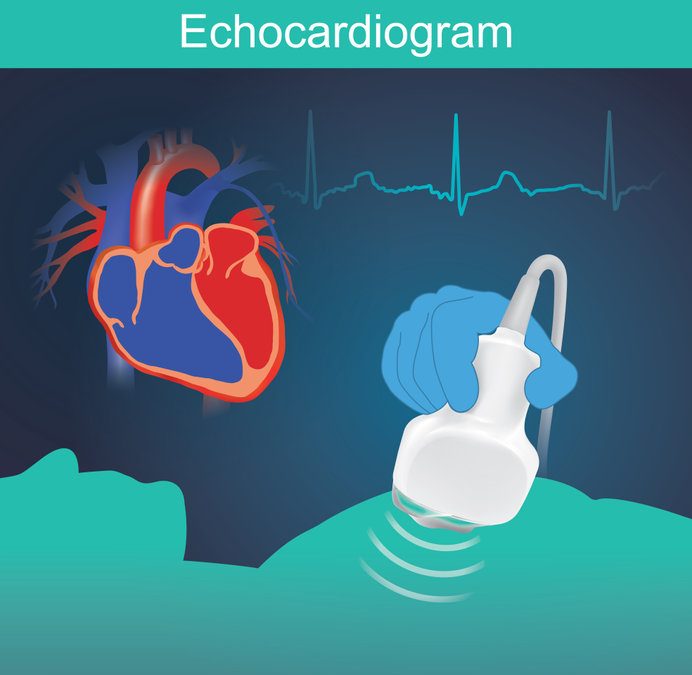
Emergency treatment for tachycardia
12th May 2022
Febrile convulsions in children
23rd May 2022Cardiac tamponade emerges when there is a fluid build-up in the space surrounding the heart but constrained by the pericardial membrane, a relatively thick and unyielding structure. This puts external pressure on the heart and reduces its ability to pump effectively. It can come about as a result of various health issues such as trauma, infection, cancer, inflammation, autoimmune disease, allergic reaction and others.
The condition is life-threatening if not treated rapidly and the more acute the onset the quicker it needs to be treated . It is rare, but it can happen to anyone, so it is important to understand how to recognise and treat it when it happens.
What are the symptoms of cardiac tamponade?
Symptoms often present suddenly and very severely if the cardiac tamponade is acute. If it is subacute, the symptoms may be subtle or non-existent early on, but get worse with time.
Possible symptoms include:
- Shortness of breath
- Discomfort or pain in the chest
- Elevated heart rate
- Rapid breathing
- Lightheadedness or fainting
- Enlarged veins in the neck
- Abdominal pain in the upper right quadrant
- Swollen arms and legs
- Fever (if infection is involved)
- Upset stomach
Acute cardiac tamponade can be accompanied by a drop in blood pressure, which may lead to symptoms of shock. Cardiac tamponade symptoms may mirror those of other health concerns so diagnosis needs to be thorough.
How do you diagnose cardiac tamponade?
Medical history is an important factor in diagnosis. An examination is also required, particularly looking for a drop in blood pressure when a breath is taken that exceeds normal parameters.
Various tests can also help with diagnosis:
- Electrocardiogram (ECG) looking for irregular rhythm or reduced size of the deflection of the chest ECG leads
- Echocardiogram to visualise heart motion and any fluid build-up
- A chest X-ray that often displayed a globular heart shadow suggestive of the diagnosis
These tests can be carried out in the Emergency Department or the ward and are done if there is an acutely unwell patient with the presumed diagnosis. If the patient is less unwell and there is time other investigations may help to elucidate the anatomy of the effusion
- CT or MRI to get further visuals of the region
If the cause of the cardiac tamponade is unknown, you must work to identify what is behind it. This is particularly important if symptoms of shock are present. Consider the following to help determine the cause:
- Blood tests for infection
- Blood tests to identify metabolic problems
- Blood tests for autoimmune disease
- Analysis of the fluid from around the heart, checking for signs of infection or cancer
How to treat cardiac tamponade
The key to treating cardiac tamponade is to remove the pericardial fluid as quickly as possible. The most common method for doing this is pericardiocentesis, wherein a catheter is used to remove the fluid usually under ultrasound guidance
The pericardial sac can also be drained during surgery. When it is done this way, the surgeon may also remove some of the pericardium in order to help identify the cause of the tamponade and potentially avoid the build-up of fluid from occurring again. This is known as a pericardial window.
There is often a substantial improvement in symptoms once the excess fluid is removed and due to the non elastic nature of pericardium the amount of fluid removed may not be great . The final outcome of treatment will depend on what caused the build-up, how severe the tamponade was, how quickly it was treated and any other health problems involved.
There are several other therapies that are often used in addition to the fluid removal:
- Monitoring with serial echocardiograms
- Therapy targeting the cause of the build-up of fluid
- Pain medication
- Medicines to boost blood pressure
- Medicines to strengthen the heart beat
- Anti-inflammatories
- Blood transfusion if trauma is involved