Primary vs secondary headaches in the emergency department
3rd August 2020
Correct Diagnosis and Treatment of Hand Injuries
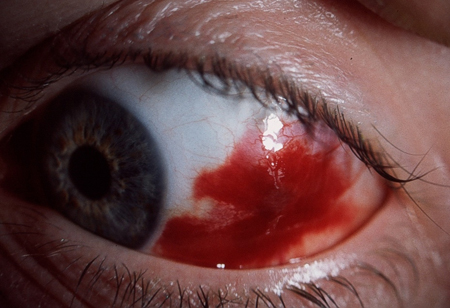
18th August 2020A foreign body (FB) in the eye usually affects the cornea or the conjunctiva. A patient presenting to the Emergency Department (ED) with this concern may be experiencing pressure, discomfort or pain in the eye accompanied by tearing, photosensitivity, excessive blinking or redness.
Most FBs that irritate the eye are inert and remain on the surface. These can usually be observed in the ED on examination. A clinician is likely to either identify the FB or see an abrasion caused by it when the foreign body has ben e removed either by blinking or tears.. The examination should be thorough, with the clinician examining the visible surface of the eye, as well as under the eyelids, where the FB may be hidden.
In certain cases, an FB can penetrate the eye; this is rare. The highest risk of this type of injury is posed by foreign objects entering the eye at a high speed, in most cases those using high speed power tools or industrial machines such as grinders
One pitfall for diagnosing this type of injury in the ED, is that a high velocity FB that has penetrated the ocular globe may not be seen on examination and indeed there may be little sings of an injury on the cornea or conjunctiva The accompanying symptoms may also differ from those present with an inert FB. A very small penetrative FB may cause few to no symptoms.
A clinician must obtain complete history to establish if and how the FB came to be in the eye. Particularly if the history of a metallic foreign body entering the eye at high speed, and the patient not wearing appropriate safety goggles should make the clinician suspect a possible penetrating injury.
In those cases an X-ray an help make the diagnosis. If there is a metallic foreign body on the surface of the eye when the patient is asked to look up and then down and 2 X-rays are taken the foreign body moves on the X-ray. If the foreign body is inside the globe of the eye there will be minimal movement of it on the X-ray when the patient looks up and down.
If an intra-ocular foreign body is not recognized in the Emergency Department and referral to the ophthalmology department is delayed there is a possibility of sight loss
Another consideration for a clinician treating a patient with a suspected, non-inert FB in the eye, whether solid or liquid, is determining whether the material may be acidic or alkalotic. These materials can cause severe injury and chemical burns and require immediate irrigation. Therefore, checking the pH level of the affected eye should be a priority; followed by irrigation of the eye until the pH has been returned to normal levels. Such irrigation may require a significant volume of fluid to be irrigated at least a few litres of saline
In conclusion, as mentioned above, most FBs in the eye are inert and remain on the surface. However, the severe, sight-threatening consequences of missing an intraocular FB necessitate that the clinician rule out worst-case scenarios first. For this reason, as is the case with many ED patients, obtaining a detailed history is essential to avoiding a missed diagnosis. A clinician must be aware of the possible signs of a corneal abrasion, an infection or a penetrating injury to the eye in order to conduct the appropriate tests and recommend correct treatment.