Saying Yes Or No To A Medico-Legal Case: Does It Matter?
6th July 2020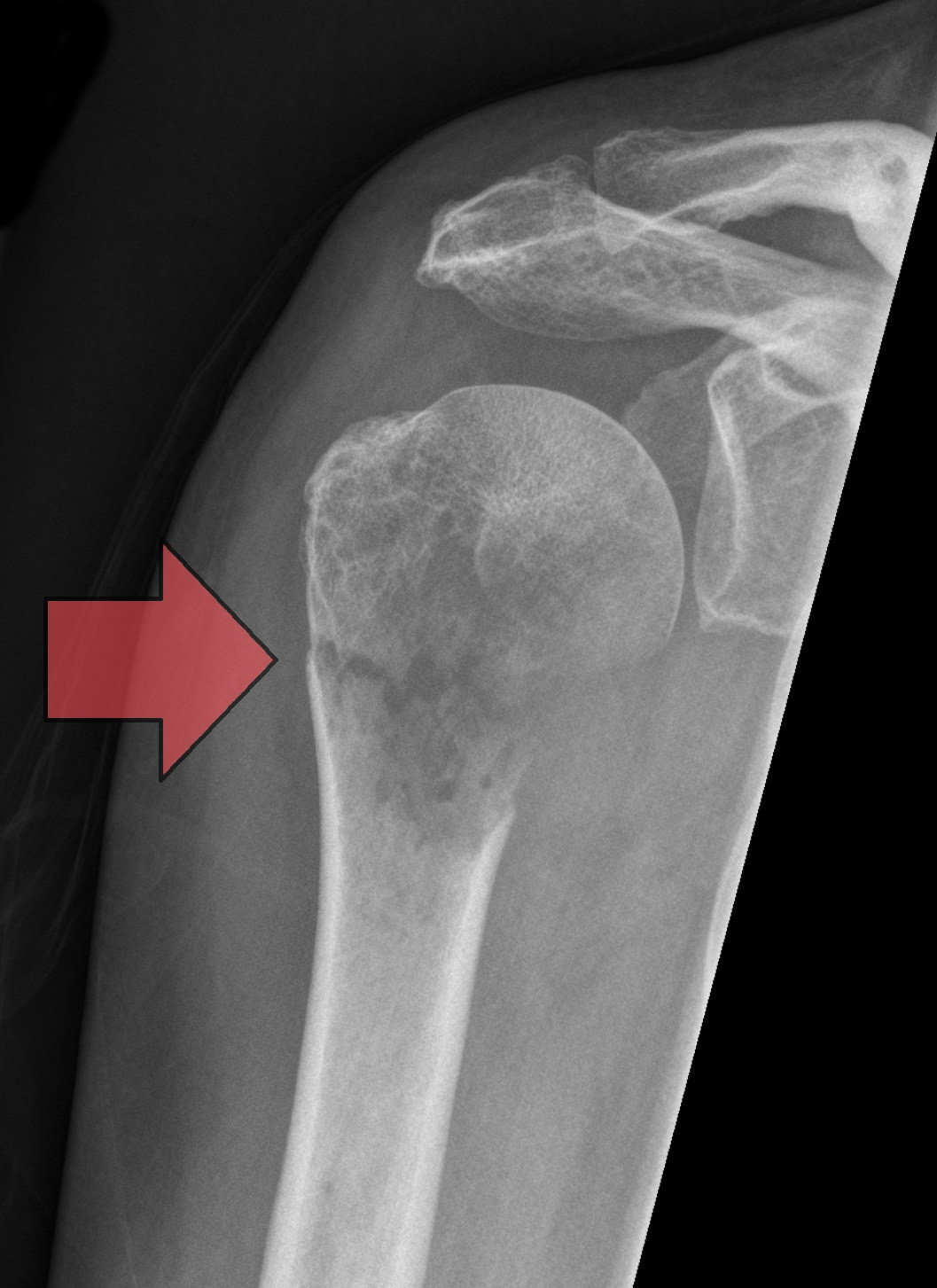
Pathological Fractures and Expert Guidelines
22nd July 2020Neck of femur fractures occur when the top part of the leg bone, just below the joint, is fractured. This is a common medical emergency among the elderly, often being caused by a fall. While less common among younger adults, it can occur in cases of high-velocity trauma or accident. (Kazley & Bagchey, 2020)
A 10-year (2005-2015) review of NHS Litigation Authority data found that the most common cause for litigation relating to hip fractures was a delay in diagnosis, which accounted for 86 claims in total (40%). (Fanous, et al., 2017) Due to the high cost in settling these cases, new national guidelines for the management of hip fractures were introduced in 2010 and 2011. These guidelines emphasise the need for quick diagnosis and early intervention when neck of femur fractures are suspected.
Complications
These fractures need to be diagnosed early and managed well to prevent serious complications. The main complications from a femoral neck fracture include non-union of the fracture or avascular necrosis (also called osteonecrosis), the death of bone tissue resulting from loss of blood supply due to the type of injury.
Differential Diagnosis
The first step in diagnosing hip fractures is to determine the cause of the injury and diagnose any potential co-morbidities. If the suspected fracture occurred due to a traumatic accident, Adult Trauma Life Support (ATLS) protocols should be followed before orthopaedic injuries are assessed. Following an initial assessment and complete history, it is necessary to determine whether a fracture exists and, if so, to understand the placement of the fracture and confirm that it is indeed a neck of femur fracture and not a fracture of the femoral head or shaft, the acetabulum or the pubic ramus.
Normally, displaced fractures present with external rotation and abduction and the affected leg may appear shorter. However, RCEM estimates that up to 15 percent of these fractures are impacted and may thus show no deformity. This is certainly one of the reasons imaging is essential for a diagnosis, as displaced fractures can be especially dangerous.
Imaging
The Royal College of Emergency Medicine (RCEM) recommends having a low threshold for conducting imaging if there is any possibility of a neck of femur fracture, especially in elderly patients presenting with hip pain after a fall. The initial recommended imaging investigations are AP pelvis and lateral of the hip radiographs.
If the X-rays do not show evidence of a fracture even after a second opinion is obtained, and the clinical symptoms persist even after analgesics are administered, an MRI may be necessary. If an MRI is not available or is contraindicated, a clinician can consider computed tomography. (NICE)
However if all the potential patient presenting with possible fractures of the neck of Femur had secondary imaging this would place a burden on both the Emergency Department and the X-ray departments and therefore some judgement is required to assess which patients would be more likely to have a fracture and therefore warrant any further imaging.
As mentioned previously in my post about indications for X-ray in fractures one of the key determinants is whether the patient can weight bear with a lower limb injury.
In the Emergency Department if the patient has a suspected fracture but the X-ray does nto show it mobilizing the patient with the help of physiotherapists if needed can be a way of reducing the need for secondary imaging if the patient can walk with minimal pain.
If they cannot this would be a good indication that they require further imaging but this may need to be arranged with an in-patient receiving team and referral to such a team from the Emergency Department can cause conflict and result in the patient being discharged without such imaging sometimes presenting later with a clinically obvious fracture that may require more extensive treatment
The life-altering complication, which can result from misdiagnosed or mismanaged neck of femur fractures, must be an essential consideration for a clinician assessing a suspected fracture of this kind. Following the national guidelines relating to management of hip fractures should prevent egregious mistakes. Conversely, for an expert evaluating a case involving this type of injury, the guidelines should serve as a foundation in determining whether the appropriate standards of care were followed.