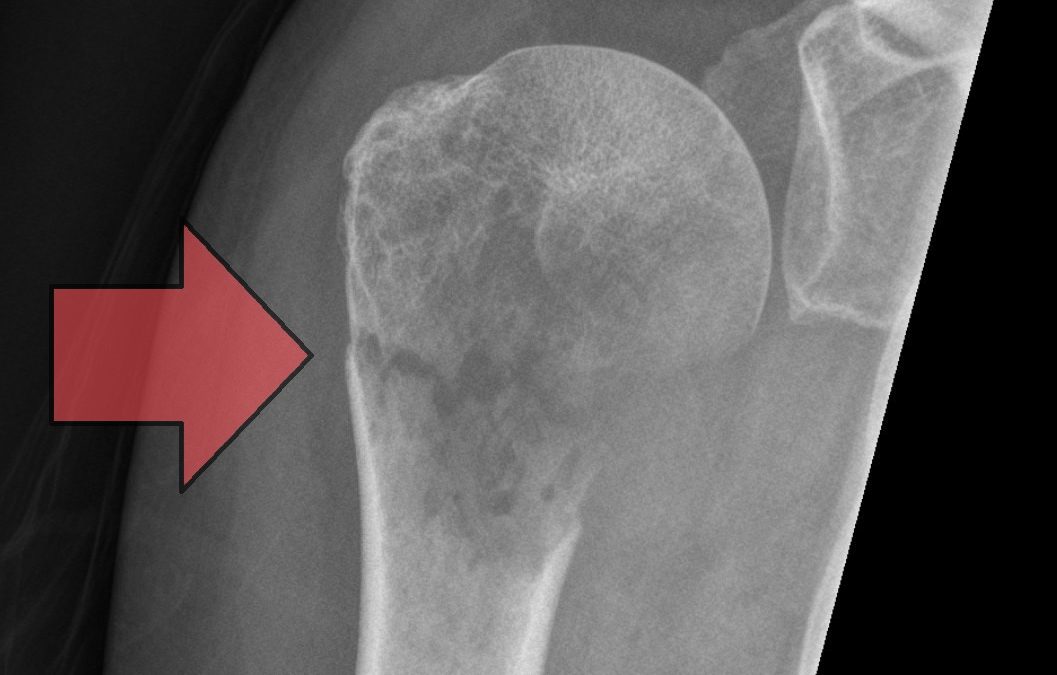
Neck of Femur Fractures in Adults
15th July 2020
Under the Microscope: the importance of meticulous record-keeping and analysis
27th July 2020I have previous written about fractures and why it is important for the clinician to assess patients fully and if required undertake imaging studies to exclude bony injury.
One of the key components in the assessment is taking a history that suggests a sufficient force has been applied to the injuries part such as to be able to cause a bony injury.
Sometimes however when taking a history the force applied to the bone may be considered by the clinician to be trivial and unlikely to cause bony damage or there is no history of a specific injury just a gradually increasing pain normally in the lower limb after an increase or unaccustomed activity.
Such a history together with signs such as point bony tenderness may be caused by pathological fractures where there is abnormal bone more susceptible to injury or a stress fracture when sub maximal forces applied constantly over a period causer micro-fractures to appear in the bone.
Pathological fractures usually occur when the bones have been weakened by pre-existing disease or infection. If the bones have been weakened, a fracture of this type can occur in the most mundane circumstances, such as sneezing or bending over. (Maurer et al. 1995)
Stress fractures, on the other hand, occur due to repeated, long-term micro-injuries to healthy bones. They are often a result of overuse, commonly from activities such as running. (Kahanov et al., 2015) During diagnosis, it is important to differentiate between the two types of fractures as that will determine the course if treatment and impact patient care and wellbeing.
Mis-diagnosed pathological fractures can be far more dangerous as the clinician will focus on measures to heal the bone, but the underlying cause of the fracture will remain unaddressed.
What are the causes of pathological fractures ?
One common cause for pathological fractures is osteoporosis, a disease that weakens the bones over time. It is more common in older adults and can often present with easily identifiable symptoms.
Osteomyelitis, a bacterial or fungal infection in the bone, can be another cause of this type of fracture. Symptoms can include fever, chills and sometimes pain, swelling or stiffness in the affected area.
Osteomalacia is yet another affliction that can lead to a fracture. It occurs when there is a Vitamin D deficiency which prevents the absorption of calcium into the bones. Signs of Osteomalacia include muscle weakness and joint pain.
Finally, a pathological fracture can be caused by a cancerous tumor. The symptoms of a tumor can vary depending on type and stage; however, this is one of the most important maladies to rule out when a pathological fracture is suspected as cancer is more treatable if caught early.
There are some other potential culprits behind a pathological fracture that may need to be considered, such as a noncancerous tumor or cyst, or the more rarely occurring diseases such as osteogenesis imperfecta (brittle bone disease) or Paget’s disease, which causes unusual bone structure. (Marshall et al., 2018)
What steps does the Emergency Medicine clinician take when presented with such an injury ?
The first part of assessment is to take a history and examine the patient and also to ask about general health and if they have any previous history of injuries with similar forces.
It is important when considering the possibility of a stress fracture to take a history of recent changed activity, such as someone starting to train for a marathon.
The key investigation is imaging again commonly plain X-ray in the first instance and these are likely to show a fracture but the quality of the bone may be abnormal, in severe cases of osteoporosis the bones may almost be invisible on an X-ray as the calcium content has reduced making the bones more radiuolucent than normal bones.
One of the key sources of error is early imaging in a stress fracture may not show any obvious fracture but if the history is suggestive of a fracture then repeating the X-ray after 10-14 days may show evidence either of a fracture or callus formation around the bone as an indirect evidence of a healing fracture.
Failing to inform the patient that if there pain persist to return for a further X-ray may cause the fracture to be missed for some time and while most of such fracture do not cause long term problems the increased pain and suffering form delayed diagnosis may lead to a claim.
While the initial way of treating the injury is in accordance with commonly accepted guideline. (such as NICE “Fractures (non-complex): assessment and management”) The difference is that once the underlying condition is identified, that will need to be managed appropriately as well. More severe fractures may require operative treatment or the need for further investigations looking for the cause of the fracture if there is localized abnormal bone where a malignant tumour is suspected.
Expert evidence
When an expert is faced with reporting on an allegation that the diagnosis was either missed or that the underlying condition was not considered they have to be mindful not only that the standard of care is that of a reasonable Emergency Medicine clinician but both the follow up arranged ( and its timeliness) or whether appropriate safety netting advice was given such that any reasonable delay in making the diagnosis was not compounded by excessive delay.