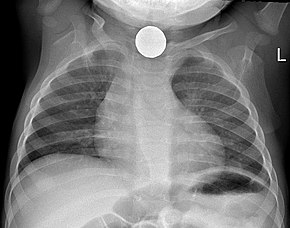
High-risk ingested or inhaled foreign bodies
17th September 2020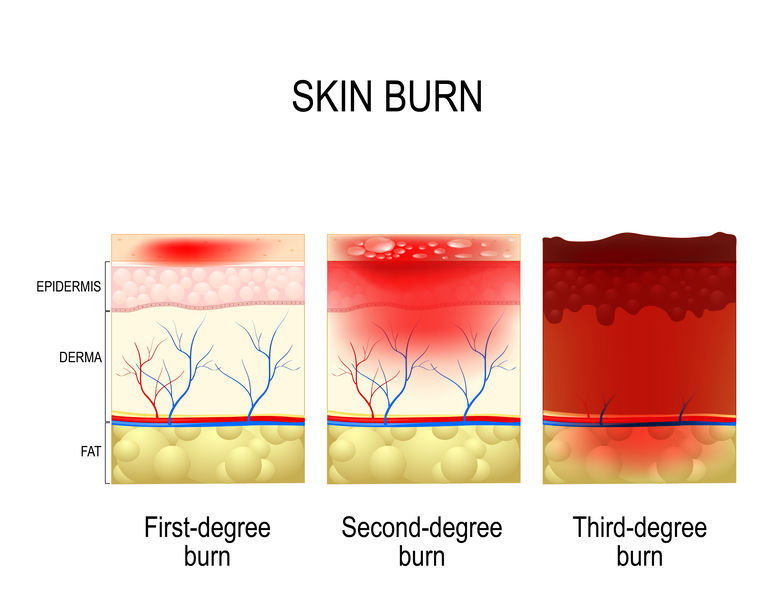
Burns pitfalls in the Emergency Department
29th September 2020Abnormal heart rates are a common presentation to the Emergency Department. In an adult the normal resting heart rate is between 60-100 beats per minute (bpm). A heart rate lower than 60 bpm is considered bradycardia and higher than 100 bpm is tachycardia. Abnormalities in the heart rhythm happen when electrical impulses in the heart become too fast, too slow, or irregular, thus causing an irregular heartbeat. The source of the irregularity can occur either in the atria (the upper chambers of the heart) or the ventricles (the lower chambers of the heart).
An abnormal heart rate may lead to poor blood circulation, as the heart’s efficiency is disrupted. Poor circulation can lead to ineffectual oxygenation, in some cases causing organ damage. In most cases abnormal heart rates are harmless, however, with some types of arrhythmias, if they are left untreated, they could lead to severe consequences and even death due to sudden cardiac arrest. It is essential for the ED clinician to be able to recognise risk factors and which cases of arrhythmia may require expert (e.g. cardiologist) consultation and further intervention.
The Resuscitation Council UK Guidelines 2015 have been accredited by the National Institute for Health and Care Excellence (NICE) and provide guidance for non-experts when diagnosing and treating arrhythmias in the ED.
Clinical presentation and initial assessment
Clinical presentations of some types of heart rate irregularities include dizziness, palpitations, pounding in the chest, fainting, shortness of breath, weakness, or fatigue. When a patient presents to the emergency department with an abnormal heart rate one of the essential skills of a clinician comes into play, the ABCDE assessment. The clinician should perform this assessment first to exclude or treat hypoxia or hypotension. Monitoring SpO2 is essential so that oxygen may be administered if patient is hypoxic. The ABCDE assessment should also help identify and treat any reversible causes of the abnormal heartrate (such as electrolyte abnormalities).
Special care should be taken if the patient is exhibiting adverse features ( e.g. shock, syncope, myocardial ischemia, heart failure) and it is suspected that the patient is at risk for cardiac arrest. Different types of arrhythmias have distinct causes and require varying levels of treatment urgency. The clinician must be able to identify the red flags and know when to escalate treatment to an expert.
Managing bradyarrhythmia
A heart rate below 60 bpm can be normal in some individuals, such as in professional athletes. The deciding factor on intervention is whether the individual is symptomatic. An otherwise healthy, asymptomatic patient likely requires no intervention. Upon initial presentation it is important that the attending physician focus on determining whether the patient is symptomatic and, if so, what is the aetiology of the symptoms.
The first diagnostic test conducted should be an ECG. Other tests should be determined by the initial assessment and suspected aetiology. Administration of atropine may be required if the patient is presenting adverse features. If the initial dose of atropine does not have the desired effect, the placement of transcutaneous pacer pads may be necessary in addition to continued pharmacological management. An expert should be consulted at this point, especially if transvenous pacing is determined to be necessary. It is important to remember that the differential diagnosis for bradycardia is broad and not all cases can be managed with vasoactive drugs and pacing. A detailed history and targeted investigations can help identify underlying pathologies in order to effectively treat symptomatic bradycardia.
Managing tachyarrhythmia
For a patient presenting with a heart rate above 100 bpm, the initial assessment is similar to the one described above. Oxygen and ECG should be monitored so that immediate concerns can be addressed. Using the ABCDE method the clinician must determine whether the patient is suffering from adverse effects. Otherwise healthy individuals are unlikely to experience adverse symptoms from arrhythmias of 100-150 bpm. The opposite is true for patients with a history of serious medical conditions such as cardiac arrest or lung disease. If the patient is unstable, synchronised cardioversion is the treatment of choice. Amiodarone should be administered if cardioversion fails.
If the patient is stable, the ECG should help the clinician determine the type of arrhythmia, which will inform treatment. The goal here is to rule out emergent, life-threatening conditions such as ventricular tachycardias or ventricular fibrillation. If other types of arrhythmia are observed and there is uncertainty, it may be necessary to involve an expert. Otherwise, once the type and cause of the arrhythmia is determined the appropriate treatment can be administered.
Conclusion
As stated above, some arrhythmias can be benign, others are known to be usually dangerous or life-threatening. Identifying the type of arrhythmia will guide the clinician in their treatment. Assessing each patient in the context of their individual circumstances and following the accepted guidelines is essential for providing the appropriate level of care.




