Arrythmias: recognising risk factors in the ED
23rd September 2020
Aortic dissection in the Emergency Department
6th October 2020In the UK, it is estimated that each year about 250,000 people with burn injuries present to primary care teams. Most likely to be affected are children under the age of 5 and the elderly over the age of 75. About 50% of burns and scalds occur in the kitchen. (Burns and scalds; NICE CKS, May 2013) Most burns are non-complex, do not require hospitalisation, and have a good prognosis. However, severe burns can lead to morbidity and death—a good outcome depends on appropriate management within the first 24 hours after the burn.
When a patient with burn injuries is admitted to the Emergency Department (ED) the burns should not be the focus of the of the initial assessment, instead the ED clinician must conduct a primary trauma survey. The patient’s airway, breathing and circulation must be thoroughly evaluated. Co-existing or related non-burn injuries or traumas that need immediate attention should be treated. Arterial blood gas determinations and baseline carboxyhaemoglobin levels should be obtained to rule out Carbon Monoxide poisoning. For patients at risk for respiratory problems who are suspected to suffer from inhalation injury, aggressive airway management with early intubation is recommended. Inhalation injuries may be hard to diagnose initially as symptoms may not be apparent for the first 24-36 hours after exposure. Thus, clinician would benefit from maintaining a high level of suspicion regarding injuries to the lungs and airways, especially when exacerbating factors, such as face and neck burns or a fire in an enclosed space, are present.
It is only after ensuring adequate airway management that the clinician should assess the severity of the burns. The key measures of burn severity include location, size, extent, and depth of the burn. Burn depth and size determine the need for fluid resuscitation.
Burn size can be assessed using the Rule of Nines (assessing body areas in multiples of 9%; head and each upper limb constitute 9% each, each lower limb, front of trunk and back of trunk represent 18%, each palmar surface, including fingers constitutes 1%.) This is different for children, for which the Lund & Browder chart can be used to assess affected area. Determining cause of burn and approximate time are essential for burn management. Fluid replacement is required for an adult with burns affecting more than 15% body surface area (excepting superficial burns); the threshold for a child is 10% of body surface. Fluid formulas (4 ml of Hartmann’s solution/kg body weight/% total body surface area) may be followed, however, these serve only as a starting point. It is recommended that urine output and end organ perfusion be measured to avoid over- and under-resuscitation.
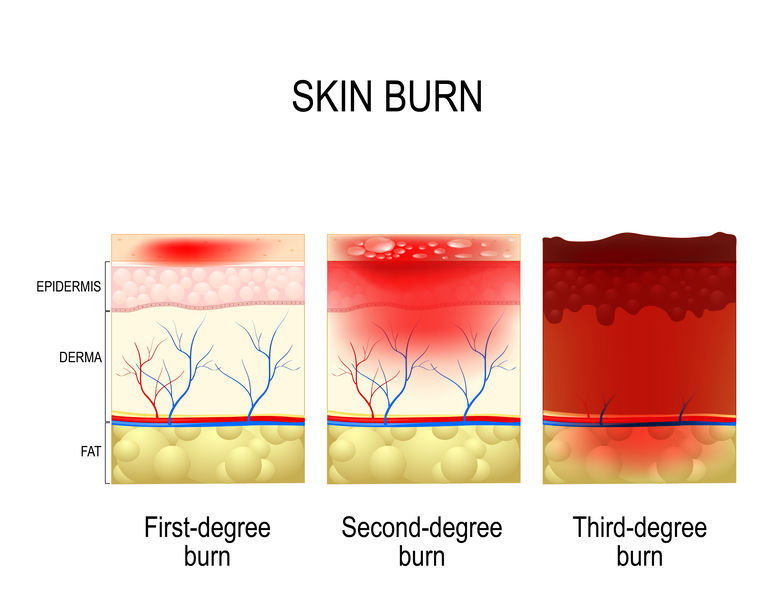
The depth of the burns can be assessed through examination by paying attention to burn erythema and sensation of the affected area. Superficial burns are usually painful, dry, red, and blanch under pressure. Partial-thickness burns usually form blisters and are painful, red, and weeping. Deeper burns are often characterised by lack of blistering, pain only when pressure is applied, and no blanching under pressure. Full-thickness burns can vary in appearance from waxy white to leathery grey to charred and black. It is important to remember that pale full-thickness burns can simulate regular skin, but are usually dry, inelastic and do not blanch when pressure is applied—a sensation may be completely absent. The depth of a burn determines the prognosis and need for surgical care. Burn depth is rarely uniform and a confounding factor is that burns are dynamic and can deepen, therefore requiring frequent reassessment. Some areas of the body where the skin is thinner are more likely to suffer deeper burns that are not initially identified as such, therefore burns to the ears, forearms, perineum and medial thighs should never be assumed to be shallow.
Superficial burns can be treated and discharged from Emergency Department. However, NICE recommends that all complex injuries should be referred to a specialist. This is especially true for patients under 5 or over 60, in addition to patients with injuries to the face, hands, perineum or any flexure, circumferential dermal burns, or a full-thickness burn of the limb, torso or neck. Inhalation injuries should be referred, as well as chemical burns affecting over 5% of the body, high-pressure steam injuries and high-tension electrical injuries. If the patient is a child, an injury should be referred if a non-accidental injury is suspected. For a patient under 16, a referral is recommended if over 5% of total body area is affected, if the patient is over 16, the tipping point is 10%. If there are serious co-morbidities, associated injuries, or pregnancy a referral should be considered.
The main takeaways for an ED clinician caring for a patient with burn injuries are as follows:
- ensure related injuries are not missed in the initial assessment;
- airway injury may not show clinical signs in the first 24 hours;
- severe burns require fluid resuscitation in appropriate quantities;
- non-painful burns are often deeper and more serious than painful ones;
- following guidelines is essential for determining when referral is necessary.