Another expert with a bill
12th October 2021
How Effective Is The New Apple Watch At Measuring Oxygen Levels?
8th November 2021Hypovolaemic shock is a medical emergency that occurs when there is a fall in circulatory volume due to a loss of blood or other body fluids. This then means that the heart is unable to pump enough blood to the body. Hypovolaemia can be difficult to diagnose and manage, and it often leads to other complications.
Causes of hypovolemia
Significant levels of blood loss are most often caused by bleeding from cuts and other injuries, internal bleeding and illness. The loss of other body fluids that result in a fall in the amount of blood circulating can be caused by vomiting, diarrhoea, burns and even excessive perspiration.
Diagnosis of hypovolaemia
Hypovolaemic shock begins to develop after 20% intravascular blood loss, which is when symptoms begin to appear. At this point, the patient is said to have entered the compensatory phase of hypovolaemia. If treatment is not successful during this stage, then the patient can enter an irreversible shock stage, leading to organ failure and death. Hypovolaemia is difficult to diagnose at this stage as blood pressure and breathing will present as normal.
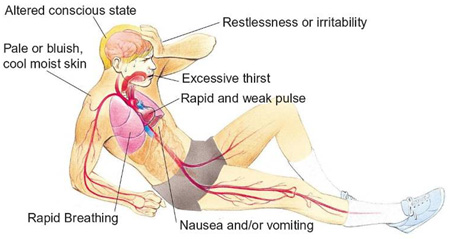
Once a patient has entered the next stage of hypovolaemic shock, when they have lost 20% to 40% blood volume, increased heart and breathing rates will usually be observed. Blood pressure might still be within normal parameters but diastolic pressure may be high. The patient may begin sweating and they could present as anxious and restless.
A patient who has lost more than 40% blood volume will experience a rapid heart rate of above 120 beats per minute with a weak pulse. Systolic blood pressure will be 100 millimetres of mercury or lower and they will be breathing rapidly; typically more than 30 breaths per minute. The patient will likely be suffering mental distress and drift in and out of consciousness. They may appear pale and sweat profusely while being cool to the touch.
Difficulties arise in determining the stage of hypovolaemia a patient has reached. Visual estimation of blood loss (VEBL) is a commonly used method to ascertain blood volume lost. This relies on a full analysis of medical history, the circumstances of the blood loss and clinical judgement. VEBL has been associated with an underestimation of blood loss in particular. A retrospective assessment may not accurately reflect the current clinical situation and lead to inconsistent management and inappropriate treatment.
Clinicians can often identify hypovolemic shock more easily when there is significant blood loss from an external wound. It can be more difficult to identify when internal bleeding occurs and when it develops from illness or an underlying medical condition. Observation and examination are used to diagnose hypovolemia. This will include blood tests and a full blood count. A CT scan of organs may also be required to identify the location of internal bleeding as well as an echocardiogram and endoscopy to indicate bleeding in the gastrointestinal tract.
Treatment of hypovolaemia
The treatment of patients with hypovolaemic shock must begin immediately by the pre-hospital care team.
One of the key changes in treatment mainly due to the military experience is that if there is severe external leading then stopping it with pressure is an immediate intervention.
This is a change in the standard ABC resuscitation algorithm to CABC.
To use a simple analogy trying to fill a bath with water without putting the plug in reminds one that giving the patient fluid without stopping the bleeding is unlikely to be successful
The patient must be transported to the emergency department as quickly as possible and it is vital that the attending trauma team is able to assess clinical presentation accurately and rapidly.
In all instances, stopping blood and fluid loss and stabilising blood volume levels are essential. Lost blood volume is usually replaced with intravenous (IV) fluids. Medicines may be required to increase blood pressure and cardiac output. Plasma and red blood cell transfusions may be required. Once blood volume levels are under control, physicians will seek to treat any underlying medical causes.
The patient’s outlook depends heavily upon rapid diagnosis and treatment and the complications that present when they are in hypovolaemic shock. Early first aid can reduce the risk of developing severe shock. The effects of shock are initially reversible but quickly become irreversible without effective treatment. Physical exam, effective consideration of medical history, identification of the cause and clinical judgement are essential for successful diagnosis and intervention.