
Testicular Torsion: Risky assumptions vs established practice
22nd June 2020
Saying Yes Or No To A Medico-Legal Case: Does It Matter?
6th July 2020A common cause for hip pain in children is transient synovitis (irritable hip), a condition usually treated with nonsteroidal anti-inflammatory drugs and rest. The main challenge to a clinician treating a child complaining of hip pain is to determine whether the pain is actually caused by a more urgent and serious condition, such as septic arthritis (an infection of the hip joint), Perthes disease (a rare childhood condition that causes inadequate blood supply to the hip) or slipped upper femoral epiphysis (SUFE, a fracture of the growth plate). All of these latter conditions may require surgical interventions and if the diagnosis is missed in the Emergency Department may lead to complications and therefore the potential for clinical negligence litigation
Determining the source of the pain
Initially, by obtaining an accurate history the clinician must rule out traumatic injury (microtrauma or repetitive trauma) as a possible cause although many patients attribute pain to a minor injury and the clinician needs to be aware of this. The clinician should conduct a thorough physical examination of the child to determine where the pain originates and to rule out confounding factors. For example, I previously wrote about testicular torsion, pain from this ailment could be referred from the groin to the hip area.
One thing to keep in mind is that hip pathology can sometimes present as knee pain, therefore when a child presents with complaints of knee joint pain, the clinician should also rule out any hip problems as illustrated in this case report by Yilmaz et al. (2011). The best way to determine if there is a significant problem in the hip is to flex and internally rotate the hip as this increases any pressure in the hip and causes pain.
Ruling out other urgent conditions
After the history has been obtained and the examination conducted, radiological investigation can usually rule out Perthes disease and SUFE. Once these two conditions have been ruled out, a clinician is left to differentiate between septic arthritis and transient synovitis, for which imaging may prove less useful. (Sultan & Hughes, 2010) This differentiation, although difficult, is crucial. Despite the fact that many studies have been conducted (Kocher et al, 1999; Caird et al, 2006) there is not an absolute set of criteria that distinguish one ailment from the other.
Transient synovitis vs septic arthritis
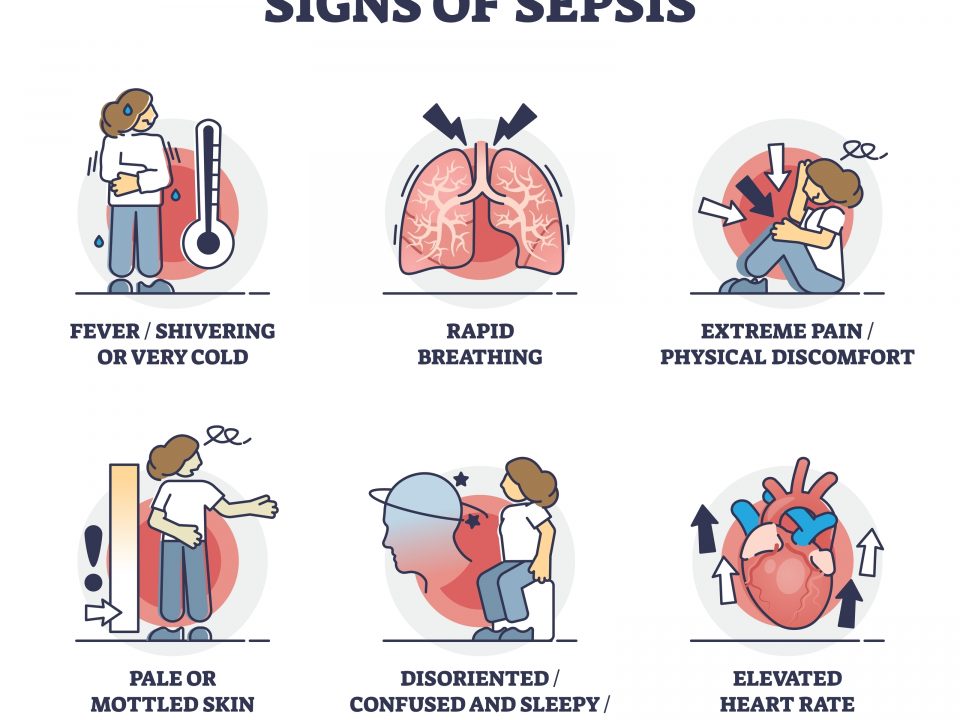
Transient synovitis and septic arthritis can present very similar symptoms early on, such as with the spontaneous onset of progressive hip, groin, or thigh pain; limp or inability to bear weight; fever; and irritability. (Houghton, 2009) Oral temperature above 38.5°C appears to be a good predictor for septic arthritis. Other indicators that could lead a clinician to suspect septic arthritis are refusal to bear weight, erythrocyte sedimentation rate more than 40 mm per hour or peripheral white blood cell count more than 12,000 per mm3 (12 × 109 per L).
If an infection is suspected, these tests should be carried out immediately. x These evidence-based clinical predictions can serve as guidelines; however, it is ultimately up to the clinician to use his or her best judgement to determine treatment.
When an expert is reviewing the care provided to a child with hip pain the care taken in recording the history and examination they performed may be the major factor is deciding whether the care the child was provided with was of a reasonable standard.



1 Comment
[…] A limp can be a secondary symptom to a wide range of other diseases and conditions. These include, but are not limited to, disorders of the abdomen, genitourinary tract, pelvis, knee, hip, foot and back. A limp could also indicate leukaemia, Perthes’ disease, slipped upper femoral epiphysis (SUFE) cerebral palsy and developmental dysplasia of the hip. A limp can also manifest in children subject to psychosocial issues. […]