
Scarcliffe V Brampton Valley Group Ltd (2023) – When Expert Witnesses Collide
29th August 2023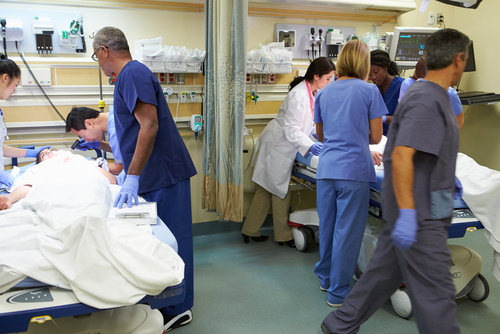
Can AI Out-perform Emergency Department Clinicians?
27th September 2023Montgomery v Lanarkshire Health Board (2015) gave rise to legal clarification on the standard of care doctors should give patients. The level of duty that a medical practitioner has is to disclose the risks of proposed treatments and to advise patients of possible alternatives. As such, doctors must show reasonable care to ensure patients are aware of their treatment and understand the risks v rewards to make an informed decision on the treatment they agree to. The judge in the case made it clear that failure to inform the patient was a breach of their duty of care and it was the court rather than the expert witnesses that made that decision about what was reasonable for a patient to be informed about.
Has The Duty To Disclose Changed?
However, there has been a recent significant judgement by the UK Supreme Court in the case of McCulloch and Others v Forth Valley Health Board. This further clarifies the extent of duty a doctor is under, as established in Montgomery.
This case sought to clarify the meaning of ‘reasonable alternative or variant treatments’, which should be a matter of judgement and professional skill by applying the Bolam test (as qualified by Bolitho) or whether such a test should be disregarded by reference to the individual patient’s circumstances and objectives.
The ruling made by the Supreme Court heard arguments from the appellant that the assessment of what is a reasonable alternative is a matter for the courts, whilst the respondent argued whether a possible treatment would be called a reasonable alternative should be one for the professional practice test. The ruling determines that a doctor will not be considered negligent if they fail to inform a patient of a treatment option if, in their opinion, the treatment is not reasonable, and an appropriate body of medical opinion would support this decision.
Personal Preference Is No Longer The Main Consideration
As such, it was confirmed that the doctor cannot simply advise a patient on treatments they personally prefer. They must identify a range of reasonable treatments and inform the patient of the risks involved unless the patient indicates otherwise. The doctor, however, is not obliged to inform patients of treatments they do not consider clinically appropriate if this would meet the professional practice test. Most importantly, this means that even if the doctor is aware of an alternative opinion after applying the professional practice test and believes it unreasonable, they are not obliged to tell the patient.
The decision is not for the court to determine, it is a matter of professional practice, and doctors should consider good practice encompassed in medical expertise. They are not obliged to discuss alternative treatments and therapies they believe to be clinically inappropriate. Such that doctors should not be placed in a position of uncertainty or conflict over applying the law and avoid the risk that the patient becomes overwhelmed and flooded with information.
How Does This Ruling Benefit Medical Professionals?
In emergency medicine, this ruling has a significant benefit. In a highly pressured medical environment where prompt action needs to be taken,treatment options may be limited, and patient awareness and approval may be a secondary consideration to keeping them alive.
Whilst doctors must be aware that good practice dictates the need to inform patients of identified alternative treatments and, in doing so, make the patient aware of the risks aligning with each course of action, it ultimately remains the decision of the medical professional to decide what those reasonable alternatives are to offer the patient. If the doctor believes that their choices would pass the professional practice test, then it is not a breach of duty of care to not inform the patient of treatments available but deemed unsuitable.
Doctors must be given a degree of protection from allegations of breach of care to deliver care that is in the best interest of patients, not simply be a conveyor of all that is possible, leaving an often confused patient to make a decision based on medical outcomes they are not fully trained to assess.




